Commercial Insurance: Premiums and Member Cost-Sharing
Key Annual Report
Commercial Insurance Premiums Finding
(Click to enlarge)
Key Annual Report
Member Cost-Sharing Finding
(Click to enlarge)
CHIA collects annual commercial health insurance premiums data from health care payers, allowing for insights into the costs borne by both Massachusetts employers and employees. CHIA also monitors high-deductible health plan enrollment and consumer cost-sharing over time. These measures are reported in CHIA's Annual Report on the Performance of the Massachusetts Health Care System.
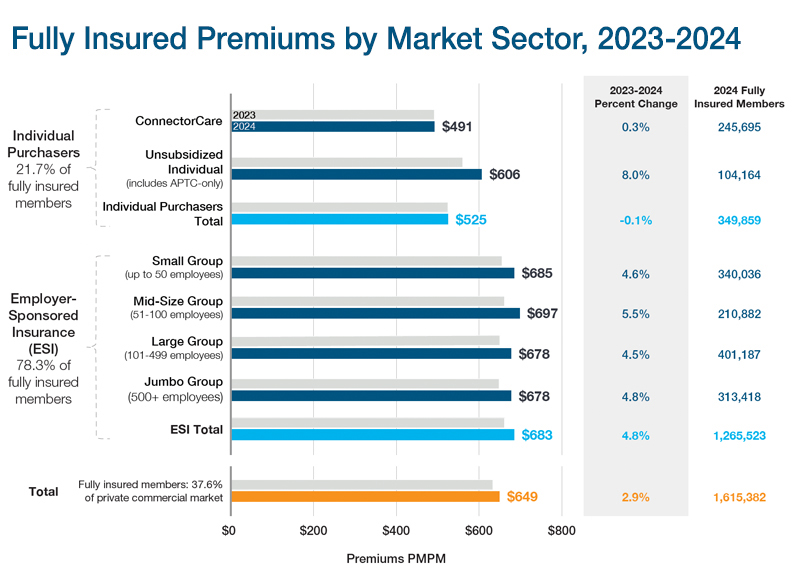
Commercial Insurance Premiums
Commercial insurance premiums are costs borne by individuals and employers. In Massachusetts, 91.9% of the commercial market is enrolled in employer-sponsored insurance, where both the employer and the employee make premium contributions to a commercial payer for an employee’s health plan. Health care payers use the premiums to pay for their members' medical expenses. Payers also retain a portion of the premium to cover administrative expenses, reserves, commissions, contributions to surpluses and profits, premium taxes, and medical management expenses.
Note that health insurance premiums are set prospectively based on historical data and projected growth in claims and administrative costs. This means that premium rates for plans active in 2024 were developed in early 2023 using historical spending data (primarily through 2022) and projected changes in utilization, unit costs, and other factors. In Massachusetts, payers are required to meet minimum medical loss ratio (MLR) thresholds of at least 88 percent in the merged market (individual purchasers and small-group employers) and 85 percent for larger employer plans. These requirements serve as guardrails to keep health plan administrative costs in check, especially in years when claims costs come in below actuarial projections.
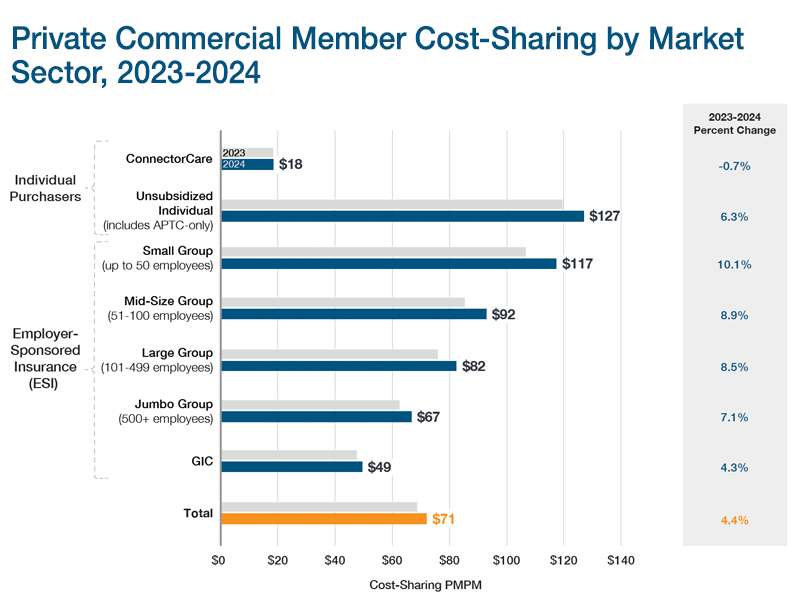
Commercial Insurance Member Cost-Sharing
Commercial insurance member cost-sharing includes all medical expenses allowed under a member’s plan but not paid for by the payer, employer, or state cost-sharing reduction (CSR) subsidies (i.e., deductibles, copays, and coinsurance). CHIA reports on member cost-sharing by market sector, product type (HMO, PPO, POS), funding type, and benefit design type (HDHP, tiered network, limited network).
Cost-sharing and affordability data are also included in findings from the Massachusetts Health Insurance Survey (MHIS) and the Massachusetts Employer Survey (MES). The MHIS findings reflect the impacts of medical costs on Massachusetts residents with all forms of insurance coverage (including private commercial, MassHealth, and Medicare) as well as the uninsured. The MES findings reflect cost-sharing and decision-making in the employer-sponsored insurance market in Massachusetts.
Note: Figures in CHIA’s Annual Report include members who incurred little to no medical costs as well as those who may have experienced substantial medical costs. They do not include out-of-pocket payments for goods and services not covered by the members’ health insurance policies (e.g., over-the-counter medicines, standalone vision and dental care). Member cost-sharing does not account for employer offsets, such as health reimbursement arrangements or health savings accounts.
Key Premiums and Member Cost-Sharing Findings
from CHIA's Annual Report on the Performance of the Massachusetts Health Care System (March 2026)
-
Fully insured premiums grew more slowly in 2024 (2.9%) than in prior years (5.9% in 2023), driven by enrollment shifts in the individual purchaser sector to lower premium ConnectorCare plans. Premiums for individual purchaser plans declined 0.1% overall, while premiums for employer-sponsored plans increased 4.8%.
-
Among small and mid-size employer groups, employers and employees faced heightened cost pressures: member cost-sharing was highest for these employees ($117 PMPM and $92 PMPM, respectively) and increased by more than 8% in 2024. These employer groups also had the highest premiums.
-
In 2024, 90.7% of premiums were used to pay for members’ medical care. The remaining 9.3% went toward non-medical expenses and payer surplus; this proportion was smaller than in the 2 prior years but similar to 2021.